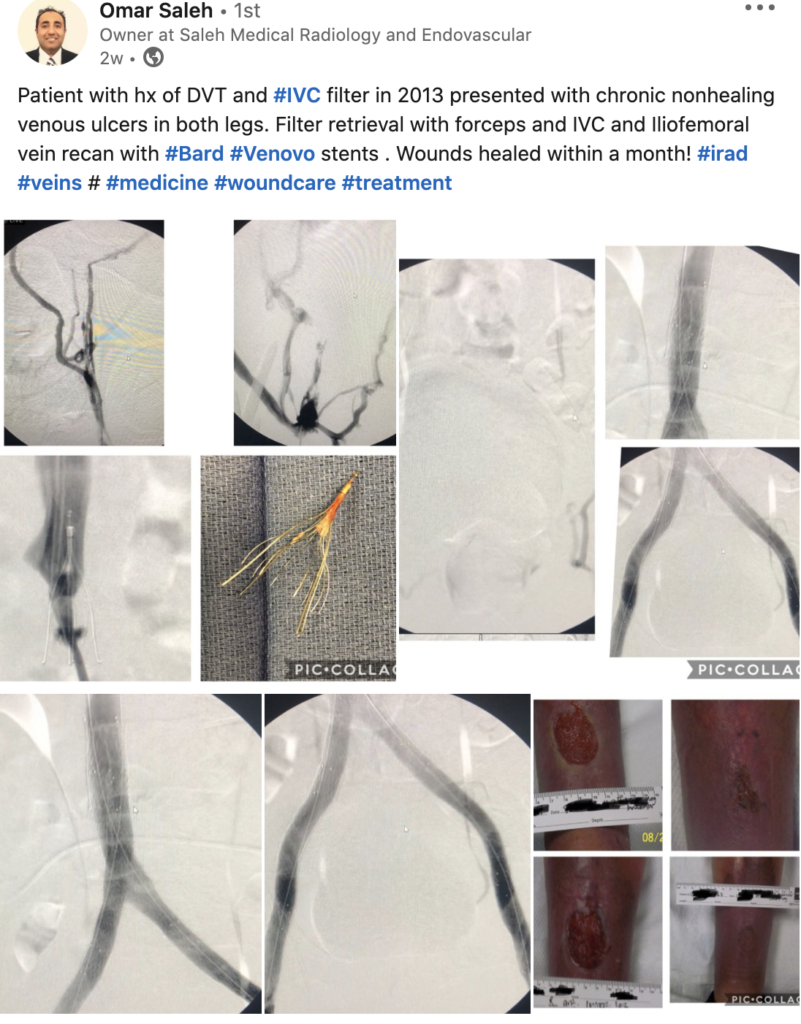
Blood clots are serious, but they are also preventable. There are several important signs and symptoms of blood clots to be on the lookout for, in addition to key risk factors to consider. Deep vein thrombosis can be very serious as blood clots in your veins can break loose, travel through your bloodstream and lodge in your lungs, blocking blood flow, and causing a potentially fatal pulmonary embolism. Veins that become blocked also may cause fluid to pool, leading to chronic venous stasis ulcers.
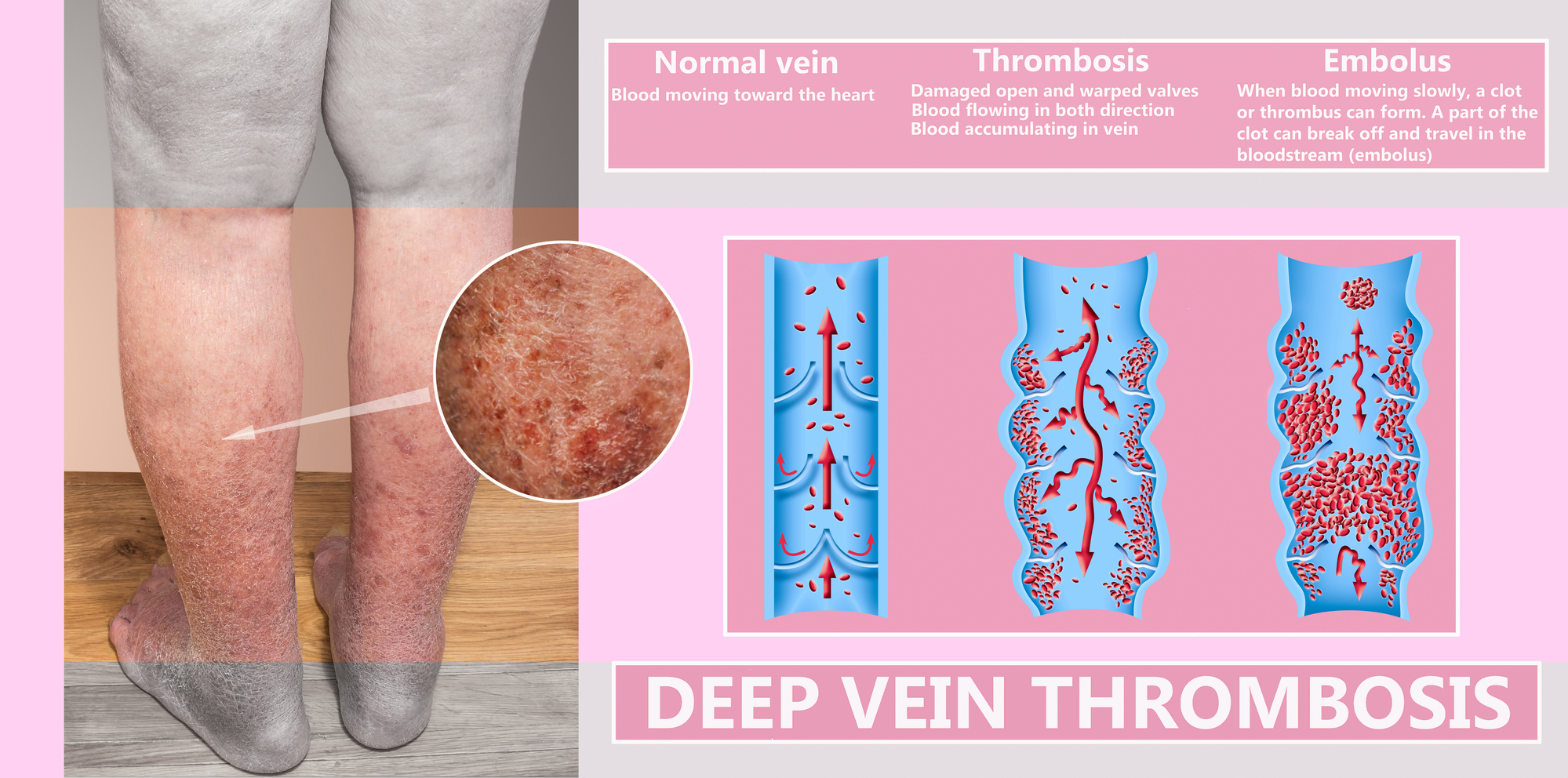
What is DVT?
If blood moves too slowly through your veins, it can cause a blood clot. Deep vein thrombosis (DVT) occurs when a blood clot forms in one or more of the deep veins in your body, usually in your legs. Deep vein thrombosis can cause leg pain or swelling, but also can occur with no symptoms.
Diagnosing DVT
When diagnosing DVT, a physician takes into consideration your specific risk factors and symptoms. A physical examination will consider other possible explanations for the symptoms and diagnostic tests can confirm through imaging of the clot. The first diagnostic method that is usually performed to image or see the clot is ultrasound.
What are Venous Ulcers?
A leg ulcer is a sore that usually develops on the inside of the leg, just above the ankle. A venous leg ulcer is the most common type of leg ulcer, accounting for more than 80% of all cases. The symptoms of a venous leg ulcer include pain, itching and swelling in the affected leg, in addition to discoloration and hardened skin around the ulcer. At times, the sore may even produce a foul-smelling discharge. DVT that develops in your legs can damage valves in the veins and increase your risk of developing venous leg ulcers.
Risk Factors
Venous ulcers are more common in women and the elderly. The primary risk factors are old age, obesity, previous leg injuries, deep venous thrombosis, and phlebitis. You’re also more at risk if you recently had an operation on your leg, such as a hip replacement or knee replacement. People with swollen and enlarged veins also have a higher risk of developing venous leg ulcers.
Other Ulcers
Neuropathic ulcers are the most common type of foot ulcers, usually caused by diabetes. Vascular disease of nerve-supplying vessels may contribute to neuropathy. The sensory component of the neuropathy results in a decreased ability to perceive pain from foreign bodies, trauma, or areas of increased pressure on the foot. Loss of sensation accompanied by trauma or increased pressure contributes to skin breakdown, often accompanied by ulcer formation at the site of pressure. These are usually arterial ulcers and these type of nonhealing wounds can lead to possible minor or major amputation of the digits, foot or leg. These can also be treated at our center.
Treatment
At the Vein & Fibroid Treatment Center, many of our patients suffer from a variety of venous conditions ranging from cosmetic spider veins to dangerous venous ulcers. Patients may suffer from deep venous thrombosis and may suffer from post thrombotic syndrome and venous ulcers. These has a huge impact on the patient’s life, their family and society. We have helped many people with chronic venous ulcers and venous hypertension, lymphedema with a venous component with venogram and angioplasty with some patients needing a stent. We use flouroscopic guidance as well Intravascular Ultrasound to treat our patients. For patients with incompetent veins and reflux we will start with a conservative measure like compression therapy. In addition to our intravascular ultrasound, we are equipped with a comprehensive x-ray at all of our centers. This enables us to diagnose and treat deep veins, which is especially important for patients with a history of DVT. To book a free screening, contact us here.
As seen on Linkedin: